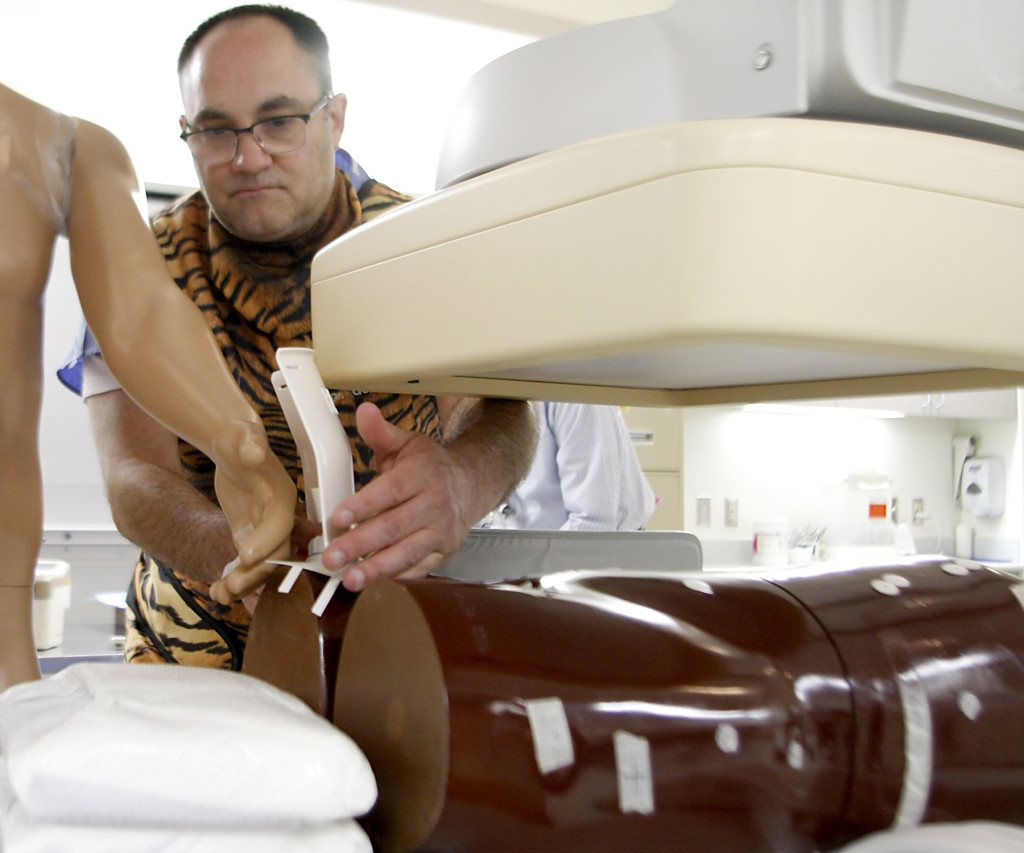
Greg Gordon, M.D., aligns a prototype of his patented Lock-Block radiation shield during a round of early tests. Dr. Gordon built his own startup company, Radux Devices, around inventions designed to better protect physicians from radiation. Photo: Charlie Litton
by Tyler Mueller, UNeMed
OMAHA, Nebraska (May 27, 2015)—A successful interventional radiology procedure can improve a patient’s life, but the people performing them, physicians like Greg Gordon, M.D., limp away feeling worse.
“I get home, and I can’t walk,” Dr. Gordon said. “I can’t move.”
Dr. Gordon invented two devices and built around them a new startup company, Radux Devices, which he hopes will make some of the pain and risk of IR a distant memory for him and other physicians. A recent proof-of-concept grant from the University’s Nebraska Research Initiative will give him the chance to prove his ideas can work.
Interventional radiologists like Dr. Gordon—who practices at Omaha’s Veteran Administration Hospital while holding a faculty appointment at the University of Nebraska Medical Center—use continuous X-ray scans to do things like injecting dyes and clearing arterial blockages through an access sheath, usually in a patient’s neck, arm or thigh.
In any IR procedure, Dr. Gordon must wear a lead-heavy protective apron that shields him from X-ray radiation. With multiple patients in a day, it’s not uncommon for physicians to wear the vest for up to 10 hours. Even with the 30-pound protective vest, X-ray radiation exposure is still a legitimate risk. And the extra weight adds bodily stress and strain that, like radiation exposure, accumulates and gets worse over time.
Bodily stress, strain, and other similar injuries are common issues, and anywhere from 60 percent to 70 percent of interventional radiologists complain about spinal problems according to a 2009 study conducted by the Society of Interventional Radiology. These injuries are caused by the leaded protection IR physicians wear while standing in awkward positions and angles. Dr. Gordon said he’s had five knee surgeries and two hip procedures to fix the damage caused—all the while suffering from an unrelated arthritic condition, ankylosing spondylitis, an inflammation of the spine where joints can fuse together.
“I think my skillsets go down because I get pain and so stressed that I can’t maintain the steady hand that I need,” Dr. Gordon said.
Besides bodily stress, cancers and tumors are another risk from IR procedures. Working closely with X-ray radiation for extended periods cumulatively increases the chances of developing health problems such as cataracts, breast cancer and central nervous system tumors, even when wearing protective garments. According to the same 2009 study, radiologists are three times more likely to die from brain cancer than physicians who do not use radiation.
Dr. Gordon said there haven’t been a lot of improvements in the health and safety for IR employees despite the risks because “that’s just part of the job.”

Lock-Block is a radiation shield that protects physicians from radiation during prodecures that require continuous x-ray imaging, such as inserting a stent. Photo: Charlie Litton
Dr. Gordon’s solutions to the problems were a flexible sheath and a radiation shield. The sheath reduces radiation exposure by pushing physicians’ hands further away from the radiation field and allowing them to operate in more comfortable positions. The portable radiation shield, about the size of a steno notebook, blocks X-ray radiation from the physician’s hands and body.
But in order for the devices to be saleable in the medical market, they need FDA approval and studies proving their effectiveness. The University of Nebraska awarded Dr. Gordon a $250,000 Nebraska Research Initiative proof of concept grant to develop and test working prototypes.











[…] 6. Radux begins prototype testing […]